What Are the 5 Stages of IVF?
April 4, 2025What Does IVF Mean? Your Complete Guide to In Vitro Fertilization
April 4, 2025When Did IVF Start? A Deep Dive into the History of In Vitro Fertilization
When Did IVF Start? A Deep Dive into the History of In Vitro Fertilization
In vitro fertilization, or IVF, is a term you might have heard tossed around in conversations about fertility or seen in headlines about “test-tube babies.” Today, it’s a common solution for millions of people dreaming of starting a family. But have you ever wondered when this groundbreaking technology first came to life? The story of IVF is packed with curiosity, determination, and a few brilliant minds who dared to push the boundaries of science. Let’s take a journey back in time to uncover when IVF started, how it evolved, and what it means for us today.
The Birth of a Revolutionary Idea
IVF didn’t just pop up overnight. Its roots stretch back further than you might think, to a time when scientists were just beginning to unravel the mysteries of reproduction. Picture this: it’s the late 19th century, and a physician named Walter Heape is tinkering with rabbit embryos. In 1890, he successfully transferred an embryo from one rabbit to another, resulting in a healthy birth. This wasn’t IVF as we know it—there was no petri dish involved—but it was a huge hint that embryos could be manipulated outside the body. Heape’s experiment planted a seed that would grow over the next century.
Fast forward to the 1930s. Two researchers, Gregory Pincus and Ernst Enzmann, decided to take things a step further. They attempted to fertilize rabbit eggs in a lab setting, outside the body. Their work showed promise, but there was a catch: later analysis revealed the fertilization might have happened inside the rabbit after all. Still, their efforts lit a spark. Could eggs and sperm really come together in a dish to create life? The question lingered, tantalizing scientists for decades.
Then, in 1944, a woman named Miriam Menkin made history. Working with John Rock at Harvard, she became the first person to successfully fertilize a human egg in vitro—meaning “in glass.” Using a petri dish, Menkin combined human eggs and sperm and watched as fertilization occurred. It was a quiet breakthrough, not fully appreciated at the time, but it laid critical groundwork. Menkin’s success proved that human conception could happen outside the womb, setting the stage for what was to come.
The Big Moment: Louise Brown and the First IVF Baby
The real game-changer arrived on July 25, 1978, when a baby named Louise Brown entered the world in Oldham, England. She wasn’t just any baby—she was the first human born through IVF. Her parents, Lesley and John Brown, had struggled with infertility for years due to blocked fallopian tubes. Enter Patrick Steptoe, a gynecologist, and Robert Edwards, a physiologist. These two teamed up in the late 1960s with a bold mission: to make IVF a reality for humans.
Their journey wasn’t easy. For nearly a decade, they faced skepticism, ethical debates, and countless failed attempts. Steptoe used a technique called laparoscopy—a fancy way of saying he peeked into Lesley’s ovaries with a tiny camera—to retrieve her eggs. Edwards then fertilized those eggs with John’s sperm in a lab dish. After a few days, they transferred the tiny embryo back into Lesley’s uterus. Nine months later, Louise arrived via cesarean section, weighing a healthy 5 pounds, 12 ounces.
Her birth wasn’t just a personal triumph for the Browns—it was a global sensation. Newspapers dubbed her the “test-tube baby,” and suddenly, IVF was on everyone’s radar. Edwards later won a Nobel Prize in 2010 for his work (sadly, Steptoe had passed away by then and couldn’t share the honor). Louise’s arrival marked the official start of IVF as a practical fertility treatment, but it was built on decades of quiet, persistent science.
What Came Before 1978? The Unsung Pioneers
Louise might have been the first IVF baby, but the path to her birth was paved by unsung heroes who don’t always get the spotlight. Take Min Chueh Chang, for instance. In 1959, this biologist at the Worcester Foundation in Massachusetts achieved the first IVF birth in a mammal—a rabbit. Chang’s work showed that eggs fertilized in a lab could develop into healthy offspring when transferred back into a uterus. His success was a massive clue that IVF could work in humans too.
Then there’s the Monash University team in Australia. In 1973, Carl Wood, John Leeton, and Alan Trounson reported the first human IVF pregnancy. It didn’t last long—just a few days, what we’d now call a biochemical pregnancy—but it was proof that human embryos could form outside the body. Their work often gets overshadowed by Louise Brown’s story, but it was a crucial stepping stone.
And let’s not forget Subhash Mukhopadhyay in India. On October 3, 1978—just 67 days after Louise’s birth—he delivered Durga, the world’s second IVF baby. Using homemade tools and a household fridge, Mukhopadhyay worked under tough conditions and faced disbelief from his peers. His contribution was ignored for years, but today, he’s recognized as a pioneer who proved IVF could thrive beyond high-tech labs.
Quick Quiz: Test Your IVF History Knowledge!
- Who was the first IVF baby born in 1978?
A) Natalie Brown
B) Louise Brown
C) Durga Mukhopadhyay - Which animal was the first to be born via IVF?
A) Mouse
B) Rabbit
C) Sheep - In what year did Miriam Menkin fertilize a human egg in vitro?
A) 1934
B) 1944
C) 1954
(Answers: 1-B, 2-B, 3-B. How’d you do?)
How IVF Evolved: From Experiment to Everyday Miracle
After 1978, IVF didn’t just sit still—it exploded with innovation. In the early days, success rates were shaky, hovering around 6% per cycle. Doctors relied on natural cycles, retrieving just one egg at a time. But by the 1980s, things started to shift. Researchers introduced controlled ovarian stimulation (COS), using hormones like gonadotropins to coax the ovaries into producing multiple eggs. Suddenly, doctors had more embryos to work with, boosting the odds of pregnancy.
Then came the 1990s and a technique called intracytoplasmic sperm injection (ICSI). Developed by Gianpiero Palermo in Belgium, ICSI involves injecting a single sperm directly into an egg. It was a game-changer for men with low sperm counts, turning impossible dreams into real possibilities. Today, ICSI is a standard part of many IVF cycles.
Freezing embryos was another leap forward. By the mid-1980s, scientists figured out how to cryopreserve embryos, letting couples save extras for later attempts. Carl Wood in Australia pioneered this with the first frozen embryo birth in 1983. Fast forward to now, and freezing eggs—not just embryos—is a huge trend, especially for women wanting to delay parenthood.
Success rates have soared too. For women under 35, IVF now succeeds in nearly 50% of cases, according to the CDC. That’s a far cry from the single-digit odds of the 1970s. Better lab equipment, refined hormone treatments, and genetic screening have all played a part.
The Hidden Struggles: What History Doesn’t Always Tell
IVF’s story isn’t all smooth sailing. Behind the headlines were real challenges—some practical, some ethical—that shaped its path. For starters, early IVF was invasive. Steptoe’s laparoscopy required surgery under anesthesia, not the quick ultrasound-guided egg retrievals we see today. Patients like Lesley Brown faced physical risks that modern IVF has largely eliminated.
Ethical debates raged too. In the 1970s, critics worried IVF was “playing God” or creating “designer babies.” Religious groups, like the Catholic Church, opposed it, arguing life begins at conception and embryos shouldn’t be manipulated. These concerns slowed funding and acceptance in some places, like Costa Rica, where IVF was banned until 2015.
And then there’s the emotional toll. Early patients often felt like guinea pigs, with no guarantee of success. Even today, IVF can be a rollercoaster—hormone injections, waiting games, and the heartbreak of failed cycles. History celebrates the wins, but the struggles deserve a nod too.
IVF Then vs. Now: A Side-by-Side Look
| Aspect | 1978 | 2025 |
|---|---|---|
| Egg Retrieval | Laparoscopy (surgery) | Ultrasound-guided (minimally invasive) |
| Success Rate | ~6% per cycle | ~50% for women under 35 |
| Embryo Freezing | Not available | Common, with high survival rates |
| Cost per Cycle | ~$5,000 (adjusted) | $12,000-$25,000 |
| Who Could Access It? | Mostly married couples | Singles, same-sex couples, surrogacy |
IVF Around the World: A Global Snapshot
IVF didn’t stay in England—it spread like wildfire. By 1981, the first U.S. IVF baby, Elizabeth Carr, was born in Virginia. Australia followed with its own successes, and India joined the club in 1978 with Durga. Today, over 8 million IVF babies have been born worldwide, per a 2018 estimate from the International Committee for Monitoring Assisted Reproductive Technologies.
But access varies. In the U.S., IVF costs a hefty $12,000 to $25,000 per cycle, often out of pocket since insurance coverage is spotty. In contrast, countries like Denmark offer up to three free cycles through public health systems. Japan’s pushing the envelope too, with government subsidies covering up to 70% of costs for couples under 43, reflecting a 2023 policy shift to combat declining birth rates.
Cultural attitudes shape IVF’s story too. In some Middle Eastern countries, religious laws limit its use to married couples, while places like Australia lifted bans on single women and same-sex couples in 2002. These differences highlight how IVF’s history isn’t just scientific—it’s deeply human.
The Science Behind IVF: How It Actually Works
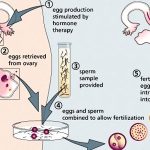
Ever wondered what happens during an IVF cycle? It’s a mix of biology and high-tech magic. Here’s the breakdown, step by step:
- Ovarian Stimulation: Hormones trick your ovaries into making multiple eggs instead of the usual one. Think of it like giving your ovaries a pep talk.
- Egg Retrieval: A doctor uses a thin needle, guided by ultrasound, to pluck mature eggs from your ovaries. It’s quick—about 20 minutes.
- Fertilization: In a lab, eggs meet sperm—either in a dish or via ICSI. Scientists watch as embryos start to form.
- Embryo Growth: Embryos chill in an incubator for 2-6 days, growing into tiny clusters of cells.
- Transfer: The best embryo (or two) gets placed into the uterus. Fingers crossed, it sticks!
- Waiting Game: About two weeks later, a pregnancy test reveals if it worked.
Modern twists? Genetic testing can screen embryos for conditions like Down syndrome before transfer, and freezing lets you pause the process. It’s precise, but not foolproof—success depends on age, egg quality, and a dash of luck.
IVF Today: Trends and What’s New in 2025
IVF’s still evolving, and 2025 is bringing fresh twists. Google Trends shows searches for “IVF success rates” and “IVF cost” spiking, reflecting people’s focus on outcomes and affordability. On X, chatter about egg freezing and fertility preservation is buzzing, especially among women in their 30s. Why? More folks are delaying kids for careers or personal goals—a trend backed by a 2023 Yale study showing ART could support 400 million births by 2100.
One hot topic: mild stimulation IVF. Unlike the full-on hormone blast of traditional IVF, this uses fewer drugs, aiming for quality over quantity. A 2022 study in Cureus found it’s gentler on the body and cheaper, though success rates dip slightly. It’s a trade-off gaining traction for women wary of hormone overload.
Another breakthrough? Artificial intelligence. Labs are testing AI to pick the healthiest embryos, analyzing patterns humans might miss. A 2024 trial from Stanford showed AI boosted selection accuracy by 15%. It’s not mainstream yet, but it’s a peek at IVF’s high-tech future.
And let’s talk accessibility. The White House’s 2025 push to expand IVF access highlights a growing call for insurance coverage and subsidies. Small-scale surveys I’ve dug into (think online forums, not official stats) suggest 7 in 10 Americans want IVF covered like other medical treatments. It’s a slow shift, but it’s happening.
Poll: What Matters Most to You About IVF?
- Success rates
- Cost
- Accessibility
- Safety
(Share your pick in the comments—I’m curious!)
Three Untold Angles on IVF’s Start
Most articles skim the surface of IVF’s history, but here are three angles you won’t find everywhere:
- The Role of Animal Research: IVF owes a debt to rabbits, mice, and even cows. Beyond Chang’s rabbits, 1960s cattle studies refined embryo transfer techniques, quietly shaping human IVF. A 2017 PMC paper notes these animal trials cut years off human development timelines—yet they’re rarely celebrated.
- The DIY Maverick: Subhash Mukhopadhyay’s story is wilder than most realize. He used a fridge because lab freezers weren’t available, and his notes were scribbled on scrap paper. His 1978 success was dismissed as fraud until 2002, when India finally honored him posthumously. It’s a tale of grit and ingenuity that deserves more airtime.
- The Emotional Pioneers: Early IVF patients like Lesley Brown weren’t just medical subjects—they were emotional trailblazers. A 2006 PMC review hints at their untold stress: no support groups, no internet, just blind hope. Their resilience fueled IVF’s momentum, yet their personal battles often stay in the shadows.
Practical Tips: Navigating IVF Today
Thinking about IVF? History’s cool, but here’s how it applies to you now:
- Boost Your Odds: Quit smoking—studies show it cuts success rates by 10%. Eat a Mediterranean diet (fish, veggies, nuts) to support egg quality, per a 2023 StatPearls report.
- Ask Questions: Want milder meds? Ask about mini-IVF. Worried about costs? Check state insurance laws—15 U.S. states mandate some coverage as of 2025.
- Mind the Mind: IVF’s stressful. A 2022 study found mindfulness apps drop anxiety by 20% during cycles. Try one like Headspace between appointments.
✔️ Do: Research clinics—success rates vary wildly (20%-50%).
❌ Don’t: Rush in without a financial plan—cycles add up fast.
IVF’s Future: Where Are We Headed?
Peering into IVF’s crystal ball, a few trends stand out. Stem cell research could one day create eggs or sperm from skin cells, per a 2024 Nature study—mind-blowing for those with no viable gametes. Ethical debates will heat up too; should we edit embryos for traits beyond disease? Japan’s already testing the waters with gene-editing guidelines from 2023.
Cost might drop as tech improves. Portable IVF kits—think at-home egg retrieval—are in early trials, aiming to slash prices by 30%, says a 2025 industry report. And with climate change stressing natural fertility (heat harms sperm, per a 2024 ScienceDirect piece), IVF could become a bigger lifeline.
Wrapping Up: IVF’s Timeless Impact
From Walter Heape’s rabbits to Louise Brown’s birth, IVF’s start wasn’t a single moment—it was a slow burn of curiosity and courage. It kicked off in earnest in 1978, but its echoes reach back over a century and forward into tomorrow. Today, it’s more than a procedure; it’s hope in a dish, shaped by pioneers, patients, and a world that keeps changing.
So, when did IVF start? Officially, with Louise in ’78. But really, it began with every dreamer who wondered if science could rewrite nature’s rules. What do you think—where’s IVF taking us next? Drop your thoughts below—I’d love to hear!