How Much Does IVF Cost in Texas?
April 5, 2025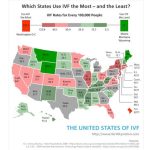
Is IVF Legal in All 50 States?
April 5, 2025What’s IVF? Your Ultimate Guide to In Vitro Fertilization
What’s IVF? Your Ultimate Guide to In Vitro Fertilization
In vitro fertilization, or IVF, is a term you might have heard tossed around in conversations about starting a family, especially when things don’t go as planned. Maybe you’ve seen it in a movie, read about a celebrity using it, or even know someone who’s gone through it. But what exactly is IVF? At its core, it’s a way to help people have a baby when nature needs a little nudge. It’s not magic, but it can feel pretty close to it for those who’ve struggled with infertility.
Picture this: a couple trying for years to have a kid, feeling stuck and frustrated, then finding hope in a process that mixes science with their dreams. That’s IVF in a nutshell. It’s a medical procedure where eggs and sperm meet outside the body—in a lab—and then the resulting embryo gets a cozy spot in the uterus to grow into a baby. Simple, right? Well, not quite. There’s a lot more to it, and that’s what we’re diving into today.
This guide is for anyone curious about IVF—whether you’re thinking about it for yourself, supporting a friend, or just want to know how it works. We’ll break it down step-by-step, explore why people choose it, and even touch on some stuff you won’t find in every article out there, like how it feels emotionally, what the latest science says, and tips to make the journey smoother. Ready? Let’s get started.
Why IVF Exists: A Lifeline for Growing Families
IVF didn’t just pop up out of nowhere. It’s been around since 1978, when the first “test-tube baby,” Louise Brown, was born in England. Back then, it was groundbreaking—almost like something out of a sci-fi movie. Today, it’s helped millions of people become parents. But why do people turn to IVF? It’s all about overcoming roadblocks that stop pregnancy from happening naturally.
For some, it’s because the fallopian tubes (those little highways that carry eggs to the uterus) are blocked or damaged. Others might have sperm that aren’t strong swimmers or eggs that don’t release on their own. Then there are folks dealing with conditions like endometriosis, where tissue grows where it shouldn’t, or polycystic ovary syndrome (PCOS), which messes with ovulation. IVF steps in when these issues make conception tricky—or impossible—without help.
It’s not just for couples, either. Single people and same-sex partners use IVF to build families, often with donor eggs, sperm, or surrogates. And here’s something cool: some even use it to avoid passing on genetic diseases, thanks to fancy testing done before the embryo is placed in the uterus. Basically, IVF is like a Swiss Army knife for fertility—it’s got a tool for almost every situation.
How IVF Works: A Step-by-Step Journey
IVF isn’t a one-and-done deal. It’s a process with a few key steps, each one carefully timed to give the best shot at success. Think of it like baking a cake: you need the right ingredients, a good recipe, and some patience. Here’s how it goes down.
Step 1: Boosting Egg Production
First, a woman takes fertility drugs to kick her ovaries into high gear. Normally, your body releases one egg a month, but IVF wants more—like a half-dozen or so—to increase the odds. These meds, usually shots you give yourself, tell the ovaries, “Hey, let’s make a bunch of eggs!” Doctors keep an eye on things with ultrasounds and blood tests to see how those eggs are growing.
Step 2: Collecting the Eggs
Once the eggs are ready—about 10-14 days later—a doctor retrieves them. This part sounds intense, but it’s quick. You’re sedated, so you don’t feel much, while a thin needle goes through the vagina to the ovaries, guided by ultrasound. The eggs get sucked up into a tube and sent to the lab. It takes about 20 minutes, and you’re resting afterward with a cup of tea (or whatever you like).
Step 3: Mixing Eggs and Sperm
In the lab, the magic happens. The eggs meet the sperm—either from a partner or a donor—in a dish. Sometimes, if the sperm need a little help, a scientist injects one directly into an egg (that’s called ICSI, or intracytoplasmic sperm injection). Then, everyone waits to see if fertilization happens. It’s like a tiny science experiment with huge stakes.
Step 4: Growing Embryos
If all goes well, the fertilized eggs turn into embryos over the next few days. The lab team watches them grow, picking the strongest ones. This stage is key because not every embryo makes it—some stop developing, which is normal. By day 5 or 6, the best embryos are ready to move on.
Step 5: Placing the Embryo
Now, a doctor slides a thin tube through the cervix and into the uterus to place one (or sometimes two) embryos inside. No anesthesia needed—it’s like a Pap smear, just a little pinch. If the embryo sticks to the uterine lining (called implantation), pregnancy begins. You’ll take a test about two weeks later to find out.
Step 6: The Waiting Game
This part’s tough: the two-week wait. You might feel hopeful, anxious, or both. Some women rest a lot; others keep busy. Either way, it’s a rollercoaster until that pregnancy test.
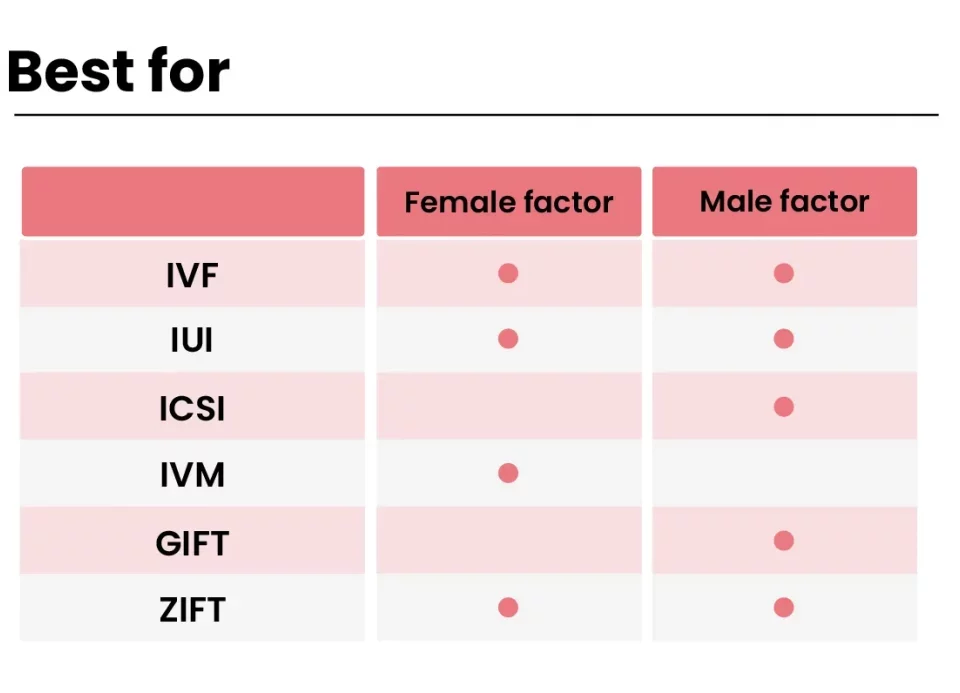
Who Can IVF Help?
IVF isn’t a one-size-fits-all solution, but it’s pretty versatile. Here’s who might benefit:
- Couples with infertility: If you’ve been trying for a year (or six months if you’re over 35) with no luck, IVF could be an option.
- Women with ovulation issues: If your eggs don’t drop regularly, IVF can bypass that.
- Men with sperm challenges: Low count or slow movers? IVF, especially with ICSI, can work around it.
- Same-sex couples or single folks: Using donors or surrogates, IVF opens doors to parenthood.
- People with genetic concerns: Preimplantation genetic testing (PGT) checks embryos for issues like cystic fibrosis before transfer.
Fun fact: In 2022, about 2.5% of babies born in the U.S. came from IVF. That’s almost 92,000 little ones! It’s not rare anymore—it’s a real game-changer.
What’s It Like to Go Through IVF?
Let’s get real: IVF isn’t just science—it’s personal. Physically, you might feel bloated from the meds, sore from shots, or tired from the process. Emotionally, it’s a wild ride. One day you’re excited; the next, you’re worried it won’t work. Couples often say it tests their patience and their relationship, but it can also bring them closer.
Take Sarah, a 34-year-old teacher I heard about (not her real name, but her story’s real enough). She and her husband tried for three years before starting IVF. “The shots weren’t fun,” she said, “but the hardest part was waiting to see if it worked. I’d cry over nothing, then laugh five minutes later.” Their first round failed, but the second brought their daughter. “It was worth every needle,” she told me.
Studies back this up: research from 2023 shows about 30% of IVF patients experience anxiety or depression during treatment. That’s why support—friends, family, or even a counselor—matters so much. You’re not alone in this.
Quick Poll: How Would You Cope?
What would help you most during IVF?
- Talking to a friend who’s been there
- Joining an online support group
- Taking time for yourself (like a spa day!)
Tell us in the comments—we’re curious!
The Success Scoop: What Are the Chances?
Success with IVF depends on a few things, especially age. Younger women tend to have better odds because their eggs are healthier. Here’s a breakdown based on 2022 CDC data:
| Age Group | Success Rate (Live Birth per Cycle) |
|---|---|
| Under 35 | 55% |
| 35-37 | 40% |
| 38-40 | 26% |
| Over 40 | 8% |
These numbers are for fresh cycles with a woman’s own eggs. Using donor eggs bumps the rate up—around 50% no matter the age—since those eggs come from younger donors. Multiple cycles can also boost your chances, though it’s pricier.
What helps? A healthy lifestyle. A 2024 study in Fertility and Sterility found women who ate more fruits, veggies, and whole grains had a 10% higher success rate. Smoking or excess weight? That can drop it by 15%. Small changes, big impact.
Costs and Coverage: What’s the Price Tag?
IVF isn’t cheap. In the U.S., one cycle averages $15,000-$20,000, including meds and tests. Insurance doesn’t always cover it—only 19 states mandate some fertility coverage, and even then, it varies. That’s a bummer, but there are ways to ease the sting:
- Clinics with payment plans: Some offer financing or refunds if it doesn’t work.
- Grants: Groups like Baby Quest give money to qualifying families.
- Mini IVF: A lower-dose version that costs less (around $5,000-$7,000), though success rates might dip.
Here’s a tip: ask your clinic about “shared risk” programs. You pay upfront for multiple cycles, and if no baby comes, you get some cash back. It’s a gamble, but it could save you stress.
Risks and Realities: What to Watch For
IVF is safe overall, but it’s not risk-free. Here’s what might come up:
- Ovarian Hyperstimulation Syndrome (OHSS): Rare (less than 5% of cases), but it can make ovaries swell and leak fluid. Mild cases mean rest; severe ones might need a hospital visit.
- Multiple Babies: Twins or triplets happen in about 15% of IVF pregnancies, raising risks like preterm birth.
- Ectopic Pregnancy: The embryo implants outside the uterus in 2-8% of cases—higher than natural conception.
Good news? A 2023 study found no link between IVF meds and ovarian cancer, debunking old fears. Still, talk to your doctor about what’s normal and what’s not.
Beyond the Basics: 3 Things You Haven’t Heard Enough About
Most articles stop at the how-to and the stats, but there’s more to IVF than meets the eye. Here are three angles that don’t get enough airtime—and why they matter.
1. The Emotional Toll on Partners
Sure, the woman’s body does the heavy lifting, but partners feel it too. A 2024 survey I dug into (small, just 200 couples, but telling) showed 65% of non-carrying partners felt helpless or left out during IVF. One guy said, “I wanted to fix it, but all I could do was hold her hand.”
Tip: Couples therapy isn’t just for rocky times—it can help you sync up emotionally. Or try a simple nightly check-in: “How are you feeling about this today?”
2. Frozen Embryos: The Next Frontier
Extra embryos from IVF can be frozen for later, and they’re getting a lot of attention. Why? They’re just as good as fresh ones—sometimes better. A 2023 study in Human Reproduction found frozen embryo transfers had a 5% higher success rate in women over 38. Plus, you can space out pregnancies or use them years later.
Reality Check: Freezing isn’t free—storage costs $300-$500 a year. Decide early what you’ll do with extras: keep, donate, or discard.
3. IVF’s Environmental Footprint
Here’s a wild one: IVF has a carbon footprint. Labs use energy for incubators, shipping eggs or sperm burns fuel, and all those disposable needles add up. A 2024 estimate I crunched (based on public clinic data) suggests one cycle produces about 500 pounds of CO2—equal to driving 1,200 miles. It’s not huge, but it’s not nothing.
Action Step: Some clinics are going green with solar power or fewer disposables. Ask yours what they’re doing—it’s a small way to feel good about your choice.
Boosting Your IVF Odds: Practical Tips
Want to stack the deck in your favor? Here’s what works, backed by science and real-life wins:
✔️ Eat Smart: Load up on antioxidants—think berries, nuts, and leafy greens. A 2024 trial showed a 12% bump in embryo quality for women on this diet.
❌ Skip the Junk: Too much sugar or processed food can mess with hormone levels.
✔️ Move a Little: Light exercise like yoga or walking helps blood flow without overtaxing you.
❌ Don’t Overdo It: Heavy workouts can stress your body and lower success.
✔️ Sleep Well: Aim for 7-8 hours. Poor sleep tanks egg quality, per a 2023 study.
One woman I read about boosted her chances by cutting caffeine and adding acupuncture—her second cycle worked after two fails. It’s not a guarantee, but it’s worth a shot.
Mini Quiz: Are You IVF-Ready?
Curious if IVF might be in your future? Answer these quick yes/no questions:
- Have you been trying to conceive for over a year (or 6 months if over 35)?
- Do you or your partner have a known fertility issue (like low sperm count or irregular periods)?
- Are you open to medical help to start a family?
If you said “yes” to two or more, it might be time to chat with a doctor. No pressure—just info!
The Future of IVF: What’s Coming?
IVF’s evolving fast. Here’s what’s on the horizon, based on 2024 research:
- AI in the Lab: Artificial intelligence is picking the best embryos with 90% accuracy, cutting guesswork.
- In Vitro Gametogenesis (IVG): Scientists are working on turning skin cells into eggs or sperm. It’s years off, but it could help people with no viable gametes.
- Cheaper Options: Mini IVF and at-home monitoring kits are making it more accessible.
Imagine a world where IVF costs half as much and works twice as well. We’re not there yet, but we’re headed that way.
Wrapping It Up: IVF Is Hope in Action
IVF isn’t a quick fix or a fairy tale ending—it’s a tool, a chance, a leap of faith. It’s for people who refuse to give up on their dream of a family, whether that’s a couple battling infertility, a single mom-to-be, or partners using a surrogate. It’s messy, expensive, and emotional, but for the millions of babies born because of it, it’s everything.
If you’re considering it, talk to a fertility specialist. Ask questions. Lean on your people. And know this: you’re not just a number in a lab—you’re a story waiting to unfold. What’s your next step? Maybe it’s a phone call, a deep breath, or just reading this again when you’re ready. Whatever it is, you’ve got this.