What Does IVF Mean? Your Complete Guide to In Vitro Fertilization
April 4, 2025Does Trump Support IVF? A Deep Dive into His Stance, Policies, and What It Means for You
April 4, 2025What Is IVF? Your Complete Guide to In Vitro Fertilization

What Is IVF? Your Complete Guide to In Vitro Fertilization
In vitro fertilization, or IVF, is a term you’ve probably heard before—maybe in a movie, a news story, or even from a friend trying to start a family. It’s one of those topics that feels both mysterious and familiar at the same time. But what exactly is IVF? At its core, it’s a way to help people have babies when nature needs a little nudge. Think of it as a bridge between hope and parenthood, built with science, patience, and a lot of heart.
IVF isn’t just one simple step—it’s a journey with twists, turns, and a mix of emotions. Whether you’re curious about how it works, wondering about the latest advancements, or just want to know what’s involved, this guide has you covered. We’ll break it down into bite-sized pieces, share some real-world insights, and even toss in a few fresh angles you won’t find everywhere else. So, grab a comfy seat, and let’s dive into the world of IVF together!
The Basics: What Does IVF Really Mean?
IVF stands for “in vitro fertilization,” a fancy Latin phrase that translates to “fertilization in glass.” Don’t worry—no one’s growing babies in test tubes! The “glass” part refers to a lab dish where sperm and eggs meet under a scientist’s watchful eye. In simple terms, IVF is a process where doctors help an egg and sperm join outside the body, then place the resulting embryo into the uterus to grow into a baby.
This isn’t how pregnancy usually happens, right? Normally, sperm and egg meet inside the body, in the fallopian tubes, and the fertilized egg travels to the uterus on its own. But for some people, that natural process hits roadblocks—maybe the tubes are blocked, the sperm can’t swim well, or the eggs aren’t releasing properly. That’s where IVF steps in, offering a detour around those obstacles.
The idea isn’t new. The first IVF baby, Louise Brown, was born in 1978 in England, and since then, millions of babies—over 8 million by some estimates—have come into the world this way. It’s become a go-to solution for infertility, but it’s also evolved into something more, helping single parents, same-sex couples, and even people who want to screen for genetic conditions.
How Does IVF Work? A Step-by-Step Breakdown
IVF isn’t a one-and-done deal—it’s a series of steps that can take weeks or even months. Each part builds on the last, like assembling a puzzle. Here’s how it unfolds:
Step 1: Boosting Egg Production
The journey starts with hormones. Women naturally release one egg a month, but IVF needs more to increase the odds of success. You’ll take daily injections or pills—think of them as a pep talk for your ovaries—to encourage them to produce several eggs at once. This stage lasts about 10-14 days, and doctors monitor you with ultrasounds and blood tests to see how those eggs are growing.
✔️ Tip: Keep a small journal to track your shots—it helps you stay organized and feel in control.
Step 2: Collecting the Eggs
Once the eggs are ready, it’s time for retrieval. This sounds scarier than it is! You’ll be under light sedation while a doctor uses a thin needle, guided by ultrasound, to gently pull the eggs from your ovaries. It takes about 20-30 minutes, and you’ll rest for a bit afterward. Most people go home the same day.
❌ Heads-Up: Don’t plan a big day after retrieval—you might feel crampy or bloated.
Step 3: Fertilizing the Eggs
Now, the lab takes over. The eggs meet the sperm in a dish, and scientists watch to see if fertilization happens. Sometimes, if the sperm needs help, they’ll use a tiny needle to inject it directly into the egg (a trick called ICSI—intracytoplasmic sperm injection). Over the next few days, the fertilized eggs grow into embryos.
Step 4: Growing Healthy Embryos
For 3-6 days, the embryos develop in a special incubator. Experts check them to pick the strongest ones—kind of like choosing the ripest fruit at the market. If you’re doing genetic testing (more on that later), this is when it happens.
Step 5: Transferring the Embryo
The big moment! A doctor uses a thin tube to place one or two embryos into your uterus. It’s quick, painless, and doesn’t need anesthesia—you’re awake the whole time. Then, you wait about 9-14 days to take a pregnancy test and see if it worked.
✔️ Pro Tip: Rest after the transfer, but don’t stress about lying flat all day—gentle movement is fine.
Step 6: Freezing Extras
If you have extra healthy embryos, they can be frozen for later. This means you could try again without starting from scratch—or even plan a sibling down the road.
Each step has its own rhythm, and the whole cycle usually takes 3-6 weeks. It’s a marathon, not a sprint, but every move gets you closer to the finish line.
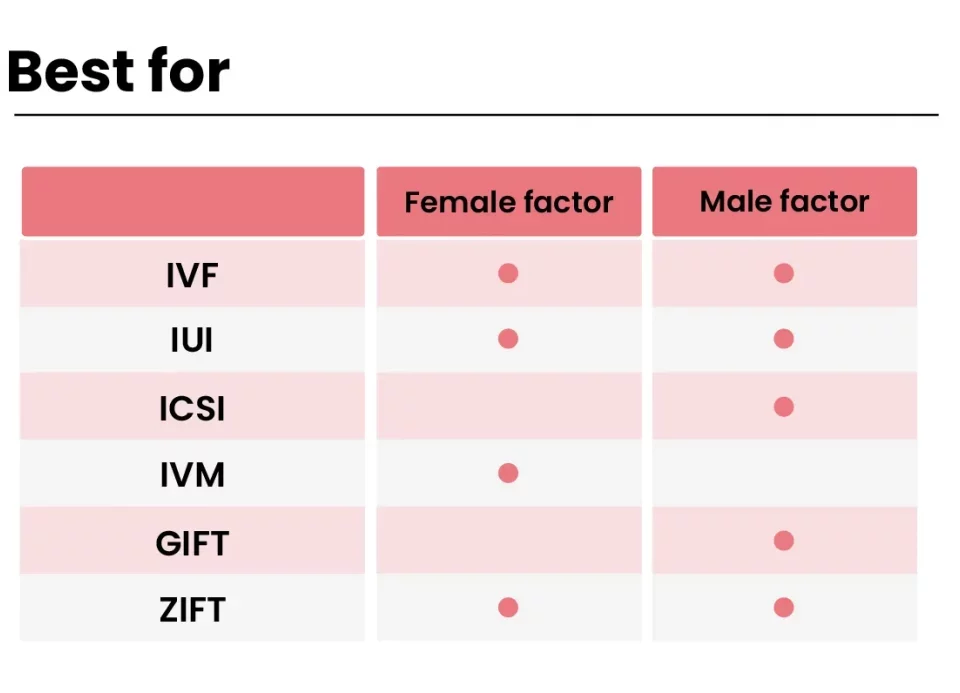
Who Needs IVF? More Than You Might Think
IVF isn’t just for one type of person—it’s a tool for all kinds of situations. Here’s who might turn to it:
- Couples with Infertility: Blocked tubes, low sperm count, or unexplained issues can make natural conception tough. IVF bypasses those hurdles.
- Single Parents by Choice: Women who want a baby on their own can use donor sperm with IVF.
- Same-Sex Couples: Gay or lesbian couples often pair IVF with donor eggs, sperm, or surrogates to build their families.
- People with Genetic Risks: If you carry a hereditary condition, IVF lets you test embryos before pregnancy to avoid passing it on.
- Older Adults: As fertility drops with age (especially after 35), IVF can help by using your eggs, donor eggs, or frozen ones from earlier years.
It’s not a one-size-fits-all fix, though. Doctors look at your health, age, and history to decide if it’s the right path. For example, someone with severe heart problems might be advised against it because pregnancy itself could be risky.
What’s New in IVF? Fresh Trends and Breakthroughs
IVF isn’t stuck in the past—it’s always evolving. Recent research and tech have brought some exciting changes that make it smarter, safer, and more accessible. Here’s what’s buzzing in 2025:
AI in the Lab
Artificial intelligence is stepping up to help pick the best embryos. Instead of relying only on a scientist’s eye, AI scans embryos for tiny details—like how fast they grow or how even their cells divide. Studies from 2023 showed AI can boost success rates by up to 15% in some cases, giving couples a better shot without extra cost.
Gentler Stimulation
Old-school IVF pumped you full of hormones, but newer “mild IVF” uses lower doses. It’s less stressful on your body and cuts the risk of ovarian hyperstimulation syndrome (OHSS), a rare but rough side effect where ovaries swell painfully. Plus, it’s cheaper—sometimes half the price of a full cycle.
Freezing Gets Better
Freezing eggs or embryos used to be tricky, but a method called vitrification (super-fast freezing) has made it nearly foolproof. More people are banking eggs in their 20s or 30s for later, and frozen embryos now have success rates almost as good as fresh ones—around 35-40% per transfer for women under 35.
Microfluidics: The Future Lab?
Imagine a tiny chip that handles the whole IVF process—egg sorting, sperm selection, and embryo growth—all in one go. This “lab-on-a-chip” idea is still in testing, but early trials suggest it could slash costs and make IVF more precise. It’s not in clinics yet, but it’s a glimpse of what’s coming.
These updates show how IVF keeps adapting to real needs—whether it’s saving money, reducing stress, or boosting odds.
The Emotional Side: What No One Tells You
IVF isn’t just about needles and lab dishes—it’s a rollercoaster of feelings. One day you’re hopeful, the next you’re anxious, and sometimes you’re just exhausted. It’s normal to feel all of that, but it’s not talked about enough.
Take Sarah, a 34-year-old teacher I heard about from a support group. She did three IVF cycles over two years. The first failed, the second ended in a miscarriage, and the third brought her daughter. She told me the hardest part wasn’t the shots—it was the waiting, the not-knowing, and the guilt when it didn’t work. “You start blaming yourself, even though it’s not your fault,” she said.
That’s why support matters. Friends, family, or even online communities can lift you up. And if it gets heavy, counselors who specialize in fertility can help you sort through the mess. One study found that people who joined support groups during IVF had lower stress levels and stuck with it longer—worth a try, right?
Quick Quiz: How Are You Holding Up?
Pause for a sec and check in with yourself:
- Do you feel hopeful about IVF, or more nervous?
- Are you talking to someone about it—partner, friend, or pro?
- On a scale of 1-5, how ready do you feel for the ups and downs?
No wrong answers—just a little nudge to think about you, not just the process.
Costs and Coverage: Breaking Down the Numbers
IVF isn’t cheap, and that’s a big worry for a lot of people. In the U.S., one cycle averages $15,000-$20,000, including meds, tests, and lab fees. Add-ons like genetic testing or freezing can bump it up another $5,000. And since it often takes more than one try—about 2-3 cycles on average for success—you could be looking at $30,000 or more.
Insurance is spotty. Only 19 states mandate some fertility coverage, and even then, IVF isn’t always included. If you’re in a state like New York or California, you might get partial help; in others, you’re on your own. Globally, places like the UK offer a few free cycles through the NHS if you’re under 40, while countries like Japan are expanding access with subsidies as birth rates drop.
Ways to Save
- Clinics with Packages: Some offer multi-cycle deals—pay upfront for 2-3 tries at a discount.
- Fertility Loans: Low-interest loans or payment plans can spread the cost out.
- Grants: Groups like Baby Quest give money to families who can’t afford IVF—apply early, though, since spots fill fast.
Here’s a quick table to compare:
| Option | Cost | Pros | Cons |
|---|---|---|---|
| Single Cycle | $15,000-$20,000 | One-time payment | Risky if it fails |
| Multi-Cycle Package | $25,000-$35,000 | Cheaper per try | Big upfront cost |
| Mini IVF (Low-Dose) | $7,000-$10,000 | Gentler, less expensive | Fewer eggs, lower odds |
Money’s a hurdle, but options are growing—especially with new tech driving costs down over time.
Risks and Realities: What to Watch For
IVF is safe for most, but it’s not risk-free. Knowing what could happen helps you prep and stay calm. Here’s the rundown:
- Ovarian Hyperstimulation Syndrome (OHSS): Too many hormones can overwork your ovaries, causing swelling or pain. It hits about 1-5% of cycles and usually fades with rest, but severe cases need a doctor.
- Multiple Births: Transferring more than one embryo raises the chance of twins or triplets—about 20% of IVF pregnancies. That’s cute but risky, with higher odds of preterm birth.
- Emotional Toll: Stress and disappointment can pile up, especially if it doesn’t work first try.
- Rare Stuff: Egg retrieval might cause bleeding or infection (less than 1%), and long-term studies on hormone use are still unfolding—no big red flags yet, though.
Success isn’t guaranteed either. For women under 35, about 50% of cycles lead to a live birth; over 40, it drops to 10-20% with your own eggs. Donor eggs or younger frozen eggs can boost those numbers, but it’s still a gamble.
✔️ Stay Smart: Ask your doc about single-embryo transfer to cut multiple-birth risks—it’s just as effective for most.
Beyond the Basics: 3 Things You Haven’t Heard Enough About
Most IVF guides stick to the usual—process, cost, success rates. But there’s more to the story. Here are three angles that deserve more spotlight:
1. The Sperm Side of Things
Eggs get all the attention, but sperm health is half the equation. Stress, diet, and even heat (think hot tubs) can tank sperm quality. A 2024 study found that men who ate more antioxidants—like berries or nuts—had better sperm motility during IVF. Yet, clinics rarely push lifestyle tweaks for guys. If you’re a couple, both of you tweaking habits could tip the scales.
✔️ Try This: Swap processed snacks for walnuts or spinach for a month before sperm collection—small changes, big payoff.
2. The Endometrium Puzzle
The uterus lining (endometrium) has to be just right for an embryo to stick. Too thin or too thick, and it’s game over. New tests like the Endometrial Receptivity Array (ERA) check if your lining’s ready, but they’re pricey and not standard yet. Some docs swear by it—others say it’s overkill. A 2023 trial showed ERA bumped success by 10% for women with past failures, so it’s worth asking about if you’ve hit dead ends.
3. Microbes Matter
Your body’s bacteria—yep, the microbiome—might play a role. Research from 2022 linked healthy vaginal and uterine microbes to better implantation rates. Antibiotics or probiotics could tweak this, but it’s early days. One clinic I read about started offering microbiome testing before IVF, claiming a 12% success boost. It’s not mainstream, but it’s a sneaky factor no one’s shouting about yet.
These nuggets show IVF’s a team sport—sperm, lining, even tiny bugs all pitch in.
Your IVF Toolbox: Practical Tips to Rock It
Ready to dive in? Here’s your starter kit—stuff you can do to feel prepared and keep your cool:
Before You Start
- Ask Questions: Write down 5 things you’re curious about (cost? risks?) and grill your doctor. No question’s too small.
- Team Up: Pick a buddy—partner, friend, or therapist—to vent to when it gets real.
- Check Your Numbers: Get a baseline on your ovarian reserve (AMH test) and sperm stats. It’s like knowing your hand before a card game.
During the Process
- Stay Chill: Yoga, walks, or even silly cat videos can ease the tension—find what works for you.
- Track Meds: Use a phone alarm or app to nail your injection times—missing one can mess things up.
- Eat Smart: Load up on protein (eggs, fish) and skip the junk—your body’s working overtime.
After the Transfer
- Rest, Don’t Freeze: Take it easy for a day, but don’t glue yourself to the couch—light activity keeps blood flowing.
- Test Wisely: Wait for the official blood test—home kits can trick you early on.
- Plan a Distraction: Binge a show or start a craft during the two-week wait—it’s a sanity saver.
Mini Poll: What’s Your IVF Game Plan?
Pick one thing you’ll try from this list—or share your own trick in your head. Little wins add up!
IVF Around the World: A Global Snapshot
IVF’s a global thing, but it looks different depending on where you are. In the U.S., it’s a private affair—lots of choice, lots of cost. In Europe, countries like Denmark lead the pack, with over 5% of babies born via IVF thanks to generous funding. Japan’s pushing it too, with new 2025 policies covering more cycles to fight a shrinking population.
Meanwhile, access lags in places like Africa or rural India, where clinics are scarce and stigma’s high. But telemedicine’s changing that—some U.S. docs now consult overseas patients online, shipping meds across borders. It’s not perfect, but it’s a start.
The Future of IVF: What’s Next?
Where’s IVF headed? Picture this: cheaper cycles, smarter labs, maybe even growing eggs from stem cells. In vitro gametogenesis (IVG)—turning skin cells into eggs or sperm—is in animal trials now. If it hits humans, it could rewrite the rules for who can have biological kids.
Cost is dropping too. Mini IVF and automation could bring prices under $10,000 soon, and groups are lobbying for universal coverage. Plus, with climate worries and delayed parenthood on the rise (hello, 30-something first-time moms), demand’s only growing—Google Trends shows “IVF cost” and “IVF success rates” spiking in 2024-2025.
Wrapping It Up: Your IVF Adventure Awaits
IVF’s more than a medical term—it’s a lifeline, a leap of faith, and a science-powered shot at a dream. From the first hormone shot to that nerve-wracking pregnancy test, it’s a wild ride with no guarantees but tons of possibility. You’ve got the basics now: how it works, who it’s for, what’s new, and how to navigate it like a pro.
But it’s not just about facts—it’s about you. Whether you’re researching for yourself, a loved one, or just to know more, you’re part of a bigger story. Millions have walked this path, and millions more will. So, take a deep breath, ask your questions, and step into it with eyes wide open. You’ve got this—and science has your back.