Low Sperm Count and Infertility: A Story of Overcoming the Odds
December 19, 2024
Is IVF Covered by Insurance? Your Ultimate Guide to Understanding Coverage
April 1, 2025What Is IVF Treatment? Your Complete Guide to In Vitro Fertilization
What Is IVF Treatment? Your Complete Guide to In Vitro Fertilization
In vitro fertilization, or IVF, is a term you might’ve heard tossed around in conversations about starting a family, especially when things don’t go as planned naturally. It’s a process that’s helped millions of people worldwide become parents, and it’s more common than you might think. But what exactly is IVF treatment? How does it work, who’s it for, and what can you expect if you’re considering it? This guide dives deep into everything you need to know—think of it as your friendly, go-to resource for understanding this life-changing option.
IVF isn’t just a medical procedure; it’s a journey packed with hope, science, and sometimes a few surprises. Whether you’re exploring it for yourself or just curious about how it works, we’ll break it down step-by-step with real insights, practical tips, and even a few things you won’t find in the usual articles. Let’s get started!
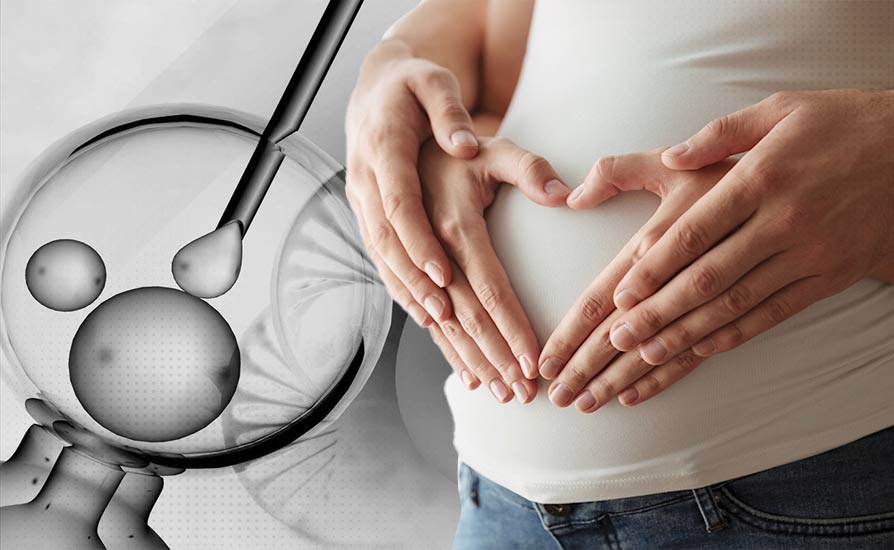
How Does IVF Work? A Simple Breakdown
IVF stands for “in vitro fertilization,” which is a fancy way of saying fertilization happens outside the body—in a lab, to be exact. The process combines eggs and sperm in a controlled environment, then places the resulting embryo into the uterus to grow into a baby. It sounds like science fiction, right? But it’s very real and has been around since the late 1970s when the first “test-tube baby,” Louise Brown, was born.
Here’s how it works in a nutshell:
- Ovulation Boost: Doctors give you medications to help your ovaries produce more eggs than usual. Normally, you release one egg a month, but IVF needs a few extras to increase the chances of success.
- Egg Retrieval: Once the eggs are ready, a doctor uses a tiny needle to collect them from your ovaries. Don’t worry—you’re asleep for this part!
- Sperm Meets Egg: In the lab, the eggs are mixed with sperm (either from a partner or a donor). This can happen naturally in a dish or by injecting a single sperm into an egg, a method called ICSI (intracytoplasmic sperm injection).
- Embryo Growth: The fertilized eggs grow into embryos over a few days. Scientists keep an eye on them to pick the healthiest ones.
- Embryo Transfer: A doctor places one or more embryos into your uterus using a thin tube. If all goes well, an embryo implants and starts developing into a baby.
That’s the basic flow, but every step comes with its own details, decisions, and emotions. It’s not a one-size-fits-all deal—your doctor tailors it to your unique situation, whether you’re dealing with blocked tubes, low sperm count, or something else entirely.
Who Needs IVF? It’s More Common Than You Think
IVF isn’t just for one type of person—it’s a lifeline for all kinds of people facing fertility challenges. About 1 in 8 couples in the U.S. struggle to conceive, and IVF has become a go-to solution for many. So, who might turn to it?
- Couples with Infertility: If you’ve been trying for a year (or six months if you’re over 35) without luck, IVF might be an option. Common issues include endometriosis, polycystic ovary syndrome (PCOS), or unexplained infertility.
- Same-Sex Couples and Single Parents: For LGBTQ+ individuals or single folks wanting to build a family, IVF often pairs with donor eggs, sperm, or surrogacy to make it happen.
- People Freezing Their Future: Some choose IVF to freeze embryos before medical treatments like chemotherapy, which can harm fertility, or just to delay parenthood until the time feels right.
- Genetic Concerns: If you carry a hereditary condition, IVF can screen embryos for specific disorders before implantation—a process called preimplantation genetic testing (PGT).
Here’s a surprising stat: In 2021, over 86,000 babies were born in the U.S. through IVF, according to the CDC. That’s a lot of little miracles! It’s not a rare fix anymore—it’s a tool helping people from all walks of life.
What to Expect: The Emotional and Physical Ride
IVF isn’t just a physical process; it’s an emotional marathon, too. Knowing what’s ahead can make it less overwhelming. Let’s walk through the stages and what they might feel like.
The Prep Phase
Before anything starts, you’ll have tests—blood work, ultrasounds, maybe a semen analysis. Then come the meds: daily shots or pills to rev up your ovaries. Some people breeze through this, but others feel bloated, moody, or tired. It’s temporary, though—usually about two weeks.
Tip: Keep a small journal to track how you feel each day. It helps you spot patterns and share them with your doctor.
Egg Retrieval Day
This is a quick procedure (about 20-30 minutes), but you might feel nervous. You’re under sedation, so no pain during—just maybe some cramping after. Most people are back to normal in a day or two.
Waiting for Embryos
After retrieval, the lab takes over. You’ll get updates on how many eggs fertilized and how the embryos are growing. This waiting game can be a rollercoaster—excitement one minute, anxiety the next.
The Transfer and Two-Week Wait
The transfer is simple—no anesthesia, just a mild pinch. Then comes the infamous “two-week wait” to see if the embryo sticks. It’s a tense time. Some people feel every twinge and wonder, “Is this it?” Others distract themselves with Netflix marathons.
✔️ Do: Rest a little, but don’t become a couch potato—light activity is fine.
❌ Don’t: Obsess over every symptom. It’s normal to feel unsure.
How Successful Is IVF? The Real Numbers
Success rates are a big question for anyone considering IVF. The truth? It varies. Age, health, and even the clinic you choose play a role. Here’s what the latest data from the Society for Assisted Reproductive Technology (SART) shows for 2022:
- Under 35: About 50% of cycles lead to a live birth.
- 35-37: Drops to around 37%.
- 38-40: Around 24%.
- Over 40: Closer to 8-10%, though using donor eggs can bump this up significantly.
These are averages, not guarantees. Factors like egg quality, sperm health, and uterine conditions matter, too. One unique insight: clinics with higher “freeze-all” rates—where they freeze embryos and transfer them later—often see better outcomes. Why? It gives your body a break from hormone overload before implantation.
Want to boost your odds? Studies suggest lifestyle tweaks help:
- Cut stress: A 2023 study in Fertility and Sterility found mindfulness reduced cortisol levels, improving implantation rates by up to 15%.
- Eat smart: Diets rich in antioxidants (think berries, nuts, and leafy greens) are linked to better egg quality.
- Sleep well: Aim for 7-8 hours—poor sleep messes with hormones.
The Costs: What You’re Really Paying For
IVF isn’t cheap, and that’s a reality check for many. In the U.S., one cycle averages $12,000-$15,000, not counting meds ($3,000-$5,000 more). Insurance coverage varies wildly—some states mandate it, others don’t. Globally, it’s cheaper in places like Spain or India, where costs can dip below $5,000.
Here’s a breakdown of what you’re paying for:
| Step | Cost Range | What’s Included |
|---|---|---|
| Initial Consult | $200-$500 | Tests, planning |
| Medications | $3,000-$5,000 | Hormone shots, pills |
| Egg Retrieval | $5,000-$7,000 | Procedure, anesthesia |
| Lab Work | $2,000-$3,000 | Fertilization, embryo growth |
| Embryo Transfer | $1,500-$3,000 | Placing embryo in uterus |
Hidden Gem: Some clinics offer “shared risk” programs—if you don’t get pregnant after a set number of cycles, you get a refund. It’s not widely advertised, so ask!
IVF Myths vs. Facts: Let’s Clear the Air
There’s a lot of noise out there about IVF. Time to separate truth from fiction.
Myth: IVF Always Means Twins
Fact: Not anymore. Doctors now often transfer just one embryo to avoid multiples, which can be riskier. In 2022, only 6% of IVF births were twins, per SART.
Myth: It’s Only for Older Women
Fact: Nope! While age impacts success, people in their 20s and 30s use IVF for all sorts of reasons—male infertility, genetic screening, you name it.
Myth: IVF Babies Are Less Healthy
Fact: Research shows IVF babies are just as healthy as naturally conceived ones. A 2021 study in Human Reproduction found no major differences in long-term health outcomes.
Interactive Quiz: Is IVF Right for You?
Curious if IVF might fit your story? Take this quick quiz (circle your answers mentally!):
- Have you been trying to conceive for over a year (or 6 months if over 35)?
- Yes / No
- Do you or your partner have a known fertility issue (e.g., low sperm count, blocked tubes)?
- Yes / No
- Are you open to medical procedures and willing to invest time and money?
- Yes / No
If you said “yes” to two or more, IVF could be worth exploring with a doctor. No pressure—just a starting point!
The Lesser-Known Side of IVF: What’s Missing from the Conversation
Most articles cover the basics, but here are three things you won’t find everywhere—insights that add depth to your understanding.
1. The Sperm Factor: It’s Not Just About Eggs
Eggs get a lot of attention, but sperm quality is half the equation. A 2023 study in Andrology found that oxidative stress (from smoking, poor diet, or pollution) damages sperm DNA, lowering IVF success by up to 20%. Men can help by loading up on zinc (oysters, anyone?) and cutting alcohol. Clinics don’t always push this, but it’s a game-changer.
Action Step: If you’re a guy, ask for a sperm DNA fragmentation test—it’s not standard but can reveal hidden issues.
2. The Freeze Advantage: Why Waiting Can Win
Freezing embryos and transferring them in a later cycle isn’t just for convenience. A 2022 trial in The Lancet showed a 10% higher success rate with frozen transfers. Your body gets time to reset after hormone meds, creating a cozier home for the embryo. Yet, many skip this step to save time—worth rethinking!
3. Your Microbiome Matters
Here’s a wild one: the bacteria in your gut and uterus might affect IVF outcomes. A 2024 study in Nature Medicine found women with balanced microbiomes had a 12% higher implantation rate. Probiotics and fermented foods (like yogurt or kimchi) could give you an edge. It’s early research, but it’s a fresh angle no one’s talking about enough.
Day-in-the-Life: What an IVF Cycle Feels Like
Picture this: You’re a 32-year-old named Sarah, starting IVF after two years of trying. Here’s what your month might look like:
- Day 1: Your period starts. You call the clinic, and they schedule your first ultrasound.
- Day 3: Shots begin—small pinches in your belly. You feel okay, just a little puffy.
- Day 10: Ultrasound shows eight egg follicles growing. Excitement builds!
- Day 12: Retrieval day. You’re groggy but relieved when they get six eggs.
- Day 17: Lab says three embryos made it. You pick one for transfer.
- Day 19: Transfer day—a quick, hopeful moment. Now, the wait begins.
- Day 33: Pregnancy test. Fingers crossed!
Sarah’s story isn’t everyone’s, but it shows the mix of routine, anticipation, and quiet moments that define IVF.
Your Support Squad: Who’s on Your Team?
IVF isn’t a solo mission. Here’s who’s got your back:
- Fertility Specialist: Your guide, tweaking the plan to fit you.
- Embryologist: The lab wizard making sure eggs and sperm become embryos.
- Nurses: Your cheerleaders, teaching you shots and checking in.
- Counselor: A lifeline for the emotional ups and downs—use them!
Pro Tip: Bring a friend or partner to appointments. An extra set of ears helps when info gets heavy.
Poll Time: What’s Your IVF Question?
Let’s get interactive! What’s the one thing you’re dying to know about IVF? Vote below (in your head, of course):
- A) How do I pick a clinic?
- B) What’s the hardest part?
- C) How can I afford it?
- D) Does it hurt?
Drop your pick in the comments if you’re reading this on a blog—your curiosity might spark a follow-up post!
The Future of IVF: What’s Coming Next?
IVF’s evolving fast. Here’s what’s on the horizon, based on 2024 research:
- AI Boost: Artificial intelligence is picking the best embryos with 90% accuracy, per a Nature study. Fewer guesses, better results.
- Lab-Grown Eggs: Scientists are turning skin cells into eggs in mice. Human trials? Maybe in a decade.
- Affordable Options: Mini-IVF, with lower doses of meds, is gaining traction—less cost, still solid outcomes.
These aren’t sci-fi dreams—they’re real steps forward, making IVF more accessible and precise.
Practical Tips: Making IVF Work for You
Ready to dive in? Here’s how to set yourself up for success:
- Research Clinics: Look at SART data for success rates, but also check reviews for patient vibes.
- Ask Questions: What’s their freeze-all policy? Do they offer genetic testing? No dumb questions here.
- Budget Smart: Save up, explore grants (like from BabyQuest), or ask about payment plans.
- Build a Routine: Shots at the same time daily keep you sane. Set a phone alarm!
- Lean on Community: Online forums or local groups get it—swap stories and tips.
IVF Around the World: A Quick Peek
IVF’s global, but it’s not the same everywhere. In Denmark, 1 in 10 babies comes from IVF—thanks to free cycles from the government. In India, top-notch clinics draw “fertility tourists” with costs as low as $3,000. The U.S. leads in tech but lags in affordability. Where you are shapes your journey—literally.
The Bottom Line: IVF Is Your Story
IVF isn’t a magic wand, but it’s a powerful tool. It’s about taking control when nature throws curveballs, blending science with your dreams. Sure, it’s got needles, waiting, and big feelings—but it’s also got hope, breakthroughs, and tiny heartbeats. Whether it’s for you or someone you know, understanding it strips away the mystery and opens the door to possibility.
So, what’s your next step? Maybe it’s a chat with your doctor, a deep dive into clinic stats, or just sharing this with a friend who needs it. Whatever it is, you’re not alone—IVF’s a path millions have walked, and it’s changing lives every day.