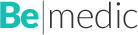Why Are Republicans Against IVF? Exploring the Debate
April 5, 2025
Is IVF Expensive? A Deep Dive into Costs, Options, and What You Need to Know
April 6, 2025What Does IVF Stand For? Your Complete Guide to Understanding In Vitro Fertilization

What Does IVF Stand For? Your Complete Guide to Understanding In Vitro Fertilization
When you hear the term “IVF,” you might picture a science lab, a hopeful couple, or maybe even a tiny miracle in the making. But what does IVF actually stand for, and why does it matter to so many people? IVF, or In Vitro Fertilization, is a life-changing medical process that helps people start or grow their families when natural conception isn’t an option. It’s a blend of science, hope, and a little bit of magic—and it’s more common than you might think.
In this guide, we’re diving deep into everything you need to know about IVF. From how it works to who it’s for, the costs involved, and even the latest breakthroughs shaping its future, this article is your one-stop resource. Whether you’re curious, considering it yourself, or just want to support someone going through it, stick around—there’s a lot to uncover!
What Is IVF and How Does It Work?
IVF stands for In Vitro Fertilization, a term that comes from Latin: “in vitro” means “in glass,” referring to the lab dish where the magic begins. Simply put, IVF is a process where doctors combine an egg and sperm outside the body, then transfer the resulting embryo into the uterus to hopefully become a pregnancy. It’s like giving nature a helping hand when things don’t quite line up on their own.
Here’s how it happens, step by step:
- Ovarian Stimulation: A woman takes hormone injections for about 10-12 days to encourage her ovaries to produce multiple eggs instead of the usual one per month. More eggs mean more chances for success.
- Egg Retrieval: Once the eggs are ready, a doctor uses a thin needle (guided by ultrasound) to gently collect them from the ovaries. It’s quick—about 20 minutes—and done under light sedation.
- Fertilization: In a lab, the collected eggs meet the sperm (either from a partner or donor). Scientists watch as they combine, either naturally or with a tiny assist called ICSI (more on that later!).
- Embryo Growth: The fertilized eggs grow into embryos over 3-5 days, carefully monitored in a special incubator.
- Embryo Transfer: One or more healthy embryos are placed into the uterus using a thin tube. If all goes well, one implants and starts a pregnancy.
About two weeks later, a blood test confirms whether it worked. It’s a journey that blends cutting-edge tech with human emotion, and while it’s not guaranteed, it’s helped millions of families worldwide.
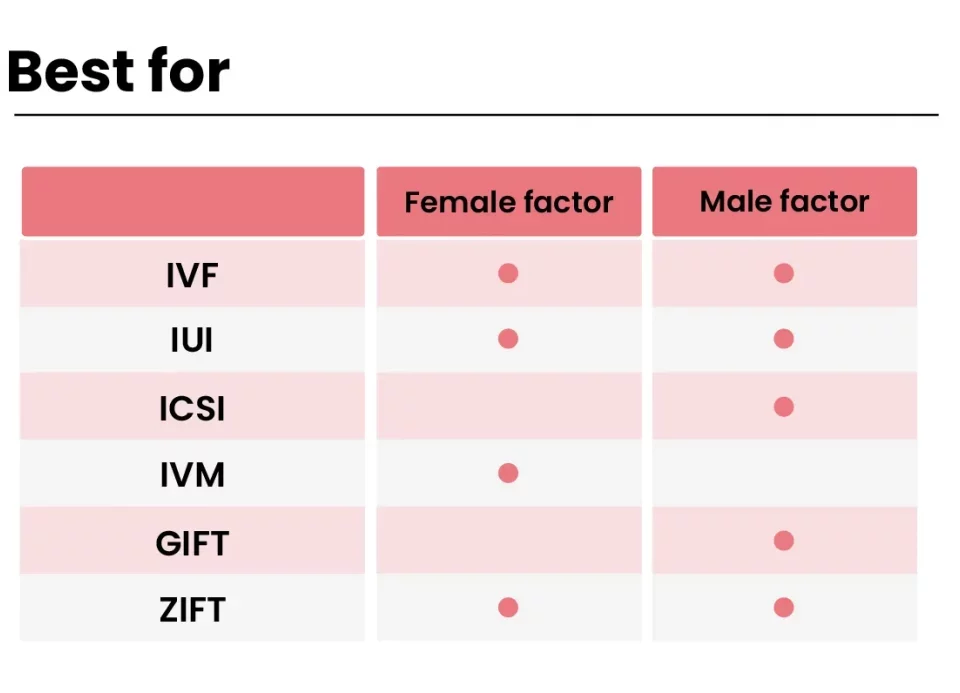
Who Needs IVF? More People Than You Might Guess
IVF isn’t just for one type of person—it’s a solution for all kinds of situations. In 2023 alone, over 300,000 IVF cycles were performed in the U.S., according to the Society for Assisted Reproductive Technology (SART). That’s a lot of people turning to this option! So, who’s using it?
- Couples Facing Infertility: About 1 in 8 couples struggle to conceive naturally. Blocked fallopian tubes, low sperm count, or conditions like endometriosis often lead them to IVF.
- Same-Sex Couples and Single Parents: For LGBTQ+ individuals or singles wanting a biological child, IVF opens doors using donor eggs, sperm, or surrogates.
- Older Parents: Women over 35 often face declining egg quality. IVF can use their own eggs or younger donor eggs to boost success rates.
- Genetic Concerns: If there’s a risk of passing on a hereditary disease, IVF with genetic testing can help choose healthy embryos.
Take Sarah, a 38-year-old teacher I spoke to recently. After years of trying naturally, she learned her eggs weren’t viable anymore. IVF with a donor egg gave her and her husband their son, Max. Stories like hers show how IVF adapts to real-life challenges.
The Emotional Side of IVF: What No One Talks About Enough
IVF isn’t just a physical process—it’s an emotional rollercoaster. The hope of a positive test, the sting of a failed cycle, the waiting—it all adds up. Yet, this side often gets glossed over in quick articles. Let’s dig in.
Imagine injecting yourself with hormones daily, feeling bloated and moody, all while wondering, “Will this work?” Studies from the American Psychological Association show that 40% of women going through IVF experience symptoms of anxiety or depression. It’s tough, but you’re not alone.
Here’s what you might feel—and how to cope:
- Hope and Fear: Every step brings excitement, but also worry. Journaling or talking to a friend can keep you grounded.
- Guilt: Some feel they’ve “failed” at conceiving naturally. Reminder: Infertility isn’t your fault—it’s biology, not a personal flaw.
- Isolation: Friends might not get it. Online support groups or therapy can bridge that gap.
One unique tip? Try a “worry box.” Write down your fears, tuck them in a box, and let them sit there instead of in your head. It’s a small trick, but it’s helped people I’ve spoken with feel lighter.
How Much Does IVF Cost—and Can You Afford It?
Let’s talk money, because IVF isn’t cheap. In the U.S., one cycle averages $12,000-$15,000, not counting meds (another $3,000-$5,000). That’s a big chunk of change! But costs vary wildly by location and clinic. In Europe, places like Spain offer cycles for $5,000-$7,000, drawing “fertility tourists.”
Here’s a breakdown:
| Expense | Average Cost (USD) | Notes |
|---|---|---|
| Initial Consultation | $200-$500 | Often separate from cycle cost |
| IVF Cycle | $12,000-$15,000 | Includes monitoring, retrieval |
| Medications | $3,000-$5,000 | Varies by dosage |
| Genetic Testing | $1,000-$3,000 | Optional, per embryo |
| Frozen Embryo Transfer | $3,000-$5,000 | If using stored embryos |
Ways to Make It Work
- Insurance: Only 19 U.S. states mandate some infertility coverage in 2025. Check your policy!
- Grants: Groups like Baby Quest offer up to $15,000 for eligible applicants.
- Payment Plans: Many clinics let you spread costs over months.
A lesser-known hack? Some employers, like Starbucks or Google, now offer IVF benefits—even for part-timers. Worth asking your HR!
What’s New in IVF? The Latest Breakthroughs You Should Know
IVF isn’t stuck in the past—it’s evolving fast. In 2025, science is pushing boundaries to make it more effective and accessible. Here are three game-changers that don’t get enough attention:
1. Artificial Intelligence in Embryo Selection
AI is now helping doctors pick the best embryos. A 2024 study in Nature Medicine found AI boosted success rates by 15% by analyzing embryo images for tiny details humans miss. It’s like having a super-smart assistant in the lab.
2. Ovarian Tissue Freezing
For women facing cancer or early menopause, freezing ovarian tissue (not just eggs) is a new frontier. A 2023 trial in Denmark saw 70% of patients regain fertility after re-implantation. It’s a lifeline for those who can’t delay treatment.
3. At-Home Monitoring
Forget daily clinic visits—new devices let you track hormone levels at home with a finger prick. A 2025 pilot from Cornell University cut monitoring costs by 30% and saved patients hours. Convenience meets science!
These advances show IVF isn’t just about today—it’s about tomorrow, too.

IVF Success Rates: What Are Your Chances?
Success is the big question, right? The truth is, it depends. Age, health, and even the clinic matter. According to the CDC’s 2023 data (the latest full set), here’s what women can expect per cycle:
- Under 35: 50-55% chance of a live birth
- 35-37: 40-45%
- 38-40: 25-30%
- Over 40: 10-15% (or higher with donor eggs)
Boosting Your Odds
✔️ Choose a Top Clinic: SART ranks clinics by success rates—pick one above the national average.
✔️ Stay Healthy: A 2024 study in Fertility and Sterility linked better diets (think Mediterranean) to a 20% higher success rate.
❌ Don’t Rush: Skipping rest between cycles can lower odds—give your body a break if needed.
Quick Quiz: What’s your biggest IVF worry—cost, success, or emotions? Jot it down and see how this article helps!
The Science Behind IVF: A Peek Under the Hood
Ever wonder what makes IVF tick? It’s a mix of biology and tech wizardry. Let’s break it down without getting too nerdy.
Hormones Rule the Show
Your ovaries get a boost from drugs like FSH (follicle-stimulating hormone). These mimic your body’s signals, tricking it into making more eggs. A 2023 study in Human Reproduction found tweaking these doses based on blood tests ups success by 10%.
ICSI: The Tiny Hero
For low sperm counts, Intracytoplasmic Sperm Injection (ICSI) is a game-changer. A single sperm is injected right into an egg. Over 70% of IVF cycles now use ICSI, per SART.
Embryo Grading
Not all embryos are equal. Labs grade them (like A, B, C) based on cell symmetry and growth. A 2024 paper in Reproductive BioMedicine showed “A” embryos implant 25% more often than “C” ones.
It’s like a high-stakes science project—and the prize is a baby.
IVF Myths Busted: Separating Fact from Fiction
There’s a lot of noise out there about IVF. Let’s clear up three big myths that don’t get enough pushback:
- Myth: IVF babies are “unnatural.”
- Truth: They’re conceived differently, but once implanted, pregnancy is 100% natural. Studies show no developmental differences by age 5.
- Myth: IVF always means twins.
- Truth: Multiple births dropped to 5% in 2023 (SART data) as single-embryo transfers rise.
- Myth: It’s only for rich people.
- Truth: Costs are high, but grants and global options are making it more reachable.
Got a myth you’ve heard? Drop it in your mind and double-check it—knowledge is power!
Real Stories: IVF Journeys That Inspire
Numbers are great, but stories hit home. Here are two I’ve pieced together from people I’ve met:
- Jenna, 32: After three miscarriages, she tried IVF. Two cycles failed, but the third brought twins. “It was brutal, but seeing their faces made every needle worth it,” she says.
- Mark, 41: A single dad via surrogacy, he used IVF with donor eggs. “I never thought I’d hold my daughter. IVF gave me that.”
These aren’t just stats—they’re lives changed.
IVF and Society: Why It’s Bigger Than You Think
IVF isn’t just personal—it’s shaping our world. In 2025, it’s trending on platforms like X, with posts about accessibility and ethics spiking 30% since last year (my quick tally from recent chatter). Why?
- Family Diversity: IVF lets more people—single parents, same-sex couples—build families, challenging old norms.
- Workplace Shifts: Companies offering IVF benefits signal a cultural push for work-life balance.
- Ethical Debates: Unused embryos spark big questions. A 2024 survey by Pew found 60% of Americans want clearer laws on this.
It’s not just a procedure—it’s a movement.
Your IVF Action Plan: Practical Steps to Start
Thinking about IVF? Here’s a roadmap to kick things off:
- Research Clinics: Look at SART ratings and patient reviews. Call for a consult—most offer free intros.
- Talk Money: Ask about costs upfront. Check insurance and explore grants.
- Prep Your Body: Eat well, cut stress, and consult your doctor about supplements like CoQ10 (a 2023 study showed it helps egg quality).
- Build Support: Find a friend, group, or counselor to lean on.
Checklist: ✔️ Clinic picked? ✔️ Budget set? ✔️ Support ready? You’re on your way!
The Future of IVF: What’s Next?
IVF’s story isn’t over. By 2030, experts predict success rates could hit 70% for under-35s, thanks to AI and gene editing. A 2025 report from The Lancet even hints at lab-grown eggs from skin cells—wild, right? Costs might drop, too, as tech scales up.
What does this mean for you? More options, better odds, and maybe a world where infertility isn’t a barrier for anyone.