How to Get IVF Covered by Insurance
April 2, 2025
Why Is IVF Controversial?
April 2, 2025How Long Does IVF Take? Your Complete Guide to the Timeline
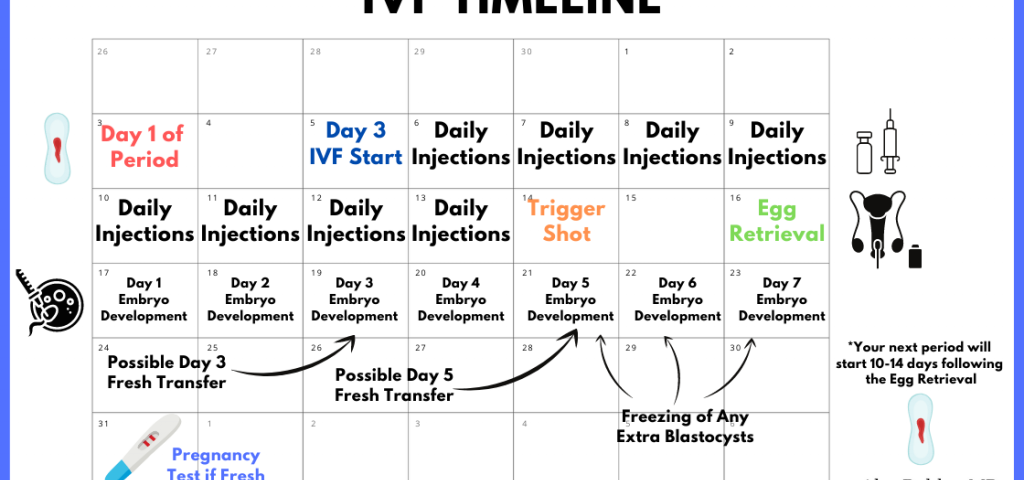
How Long Does IVF Take? Your Complete Guide to the Timeline
Starting a family can feel like a big adventure, and for some, in vitro fertilization (IVF) becomes part of that journey. If you’re wondering how long IVF takes, you’re not alone—it’s one of the first questions people ask when they’re thinking about this option. The process can seem mysterious, but it’s really just a series of steps that work together to help you grow your family. In this guide, we’ll walk you through every stage, break down the timeline, and share some practical tips to make it all feel less overwhelming. Whether you’re just curious or ready to dive in, here’s everything you need to know about how long IVF really takes—and what you can expect along the way.
What Is IVF, Anyway? A Quick Rundown
IVF is like a helping hand for people who need a little extra support to get pregnant. It’s a process where doctors take eggs from the ovaries, mix them with sperm in a lab, and then place the resulting embryo back into the uterus. Think of it as giving nature a nudge in a controlled, scientific way. It’s been around since 1978 when the first “test tube baby,” Louise Brown, was born, and today, it’s helped millions of families worldwide.
The timeline for IVF isn’t a one-size-fits-all deal—it depends on your body, your situation, and even the clinic you choose. On average, though, a single IVF cycle takes about 3 to 6 weeks from start to finish. But there’s more to it than just that window. Let’s break it down step by step so you can see the full picture.
The Big Picture: How Long Does a Full IVF Cycle Take?
A “cycle” in IVF lingo means the whole process from prepping your body to finding out if you’re pregnant. Here’s a quick snapshot of the timeline:
- Prep Phase (0-2 months): Before the cycle even starts, there’s some groundwork—like tests and planning—that can take a few weeks or more.
- Active Cycle (3-6 weeks): This is the main event, from starting meds to the pregnancy test.
- Total Time (1-3 months): Add it all up, and you’re looking at a couple of months for one shot at IVF.
But that’s just the surface. Each part has its own pace, and things like your age, health, or whether you’re using fresh or frozen embryos can shift the schedule. Let’s dive into the details.
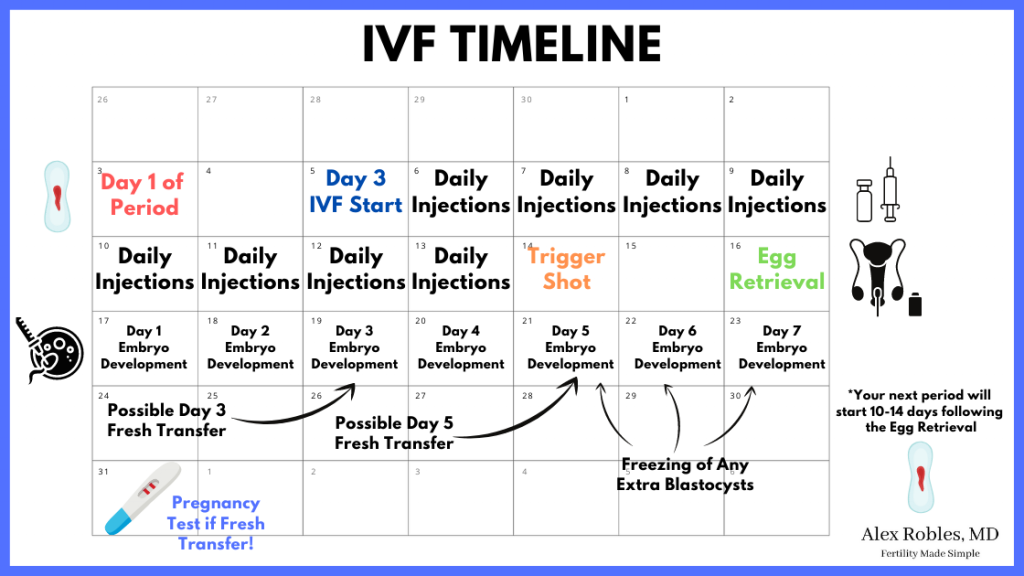
Step 1: Getting Ready—What Happens Before the Cycle Starts
Before you jump into IVF, there’s a prep phase that sets the stage. This isn’t technically part of the “cycle,” but it’s super important. It can take anywhere from a few days to 2 months, depending on your situation.
What’s Involved?
- Tests and Checkups: Your doctor will run blood tests to check your hormone levels, do an ultrasound to peek at your ovaries, and maybe even test your partner’s sperm. This helps them figure out the best plan for you.
- Consultations: You’ll sit down with your fertility team to talk about your options—like whether you’ll use your own eggs or a donor’s—and map out the timeline.
- Lifestyle Tweaks: Some clinics suggest changes like cutting back on caffeine or starting prenatal vitamins to get your body ready.
How Long Does It Take?
If everything’s straightforward, this might wrap up in a week or two. But if you need more tests—like genetic screening—or if your doctor wants to sync your cycle with a donor, it could stretch to a month or two. For example, a 2023 study from the National Institutes of Health found that pre-IVF testing can delay the start by up to 60 days for about 15% of patients due to scheduling or unexpected results.
Pro Tip:
Ask your clinic for a checklist of what’s needed upfront. Getting all your ducks in a row early can shave weeks off this phase.
Step 2: Ovarian Stimulation—Revving Up Your Ovaries
Once you’re cleared to start, the first big step is ovarian stimulation. This is where you take meds to help your ovaries make more eggs than they would on their own. It usually lasts 8 to 14 days.
How It Works
- You’ll get daily injections of hormones (like FSH or follicle-stimulating hormone) to wake up your ovaries.
- Your doctor will monitor you with ultrasounds and blood tests every few days to see how your eggs are growing.
- When the eggs are ready—usually about the size of a grape (18-20mm)—you’ll get a “trigger shot” to help them mature.
Why the Time Varies
- Your Body’s Response: Some people grow eggs fast, while others need a little longer. A 2022 study in Fertility and Sterility showed that women over 35 might need an extra 2-3 days of stimulation compared to younger patients.
- Protocol Type: There’s a “long protocol” (starting with suppression meds a few weeks earlier) or a “short protocol” (straight to stimulation). The short one’s more common and quicker.
What to Expect
You might feel bloated or moody from the hormones—totally normal! Keep a calendar handy to track your shots and appointments.
Step 3: Egg Retrieval—Harvesting the Goods
After your eggs are ripe, it’s time for retrieval. This step happens in one day, but it’s a biggie.
The Process
- You’ll go under light sedation while the doctor uses a thin needle (guided by ultrasound) to scoop out the eggs from your ovaries.
- It takes about 20-30 minutes, and you’ll rest for a couple of hours after before heading home.
Timing Details
- The retrieval is scheduled 36 hours after your trigger shot—super precise timing to catch the eggs at their peak.
- Recovery’s quick—most people are back to normal within a day or two, though you’ll want to take it easy.
Fun Fact
On average, doctors collect 8-15 eggs per retrieval, according to the American Society for Reproductive Medicine (ASRM). More eggs can mean better odds, but it doesn’t guarantee success.
Step 4: Fertilization and Embryo Growth—Lab Magic
Now the lab takes over. This phase lasts 3 to 7 days, depending on how long the embryos grow.
What Happens
- The eggs get mixed with sperm (either naturally or with a technique called ICSI, where a single sperm is injected into each egg).
- Over the next few days, the fertilized eggs become embryos. The lab watches them closely to see which ones are strongest.
- Embryos are usually transferred at day 3 (cleavage stage) or day 5/6 (blastocyst stage)—day 5 is more common now because it boosts success rates.
Why It Varies
- Embryo Quality: If you’ve got a lot of healthy embryos, the lab might wait until day 5. Fewer or slower-growing ones might mean a day 3 transfer.
- Clinic Preference: Some places stick to a set schedule, while others tailor it to you.
Cool Insight
A 2024 study from Human Reproduction found that waiting until day 5 can increase live birth rates by up to 10% compared to day 3 transfers. It’s like letting the embryos prove they’ve got what it takes!
Step 5: Embryo Transfer—Back to You
The transfer is quick and easy, taking just one day.
How It Goes
- A thin tube slides the embryo(s) into your uterus—no anesthesia needed, just a full bladder for better ultrasound visuals.
- You’ll lie down for 15-30 minutes after, then head home with fingers crossed.
Timing Twist
- If you’re doing a “fresh” transfer, it’s 3-7 days after retrieval. But if you’re freezing embryos (more on that later), this step could happen months later.
Heads-Up
Doctors usually transfer 1-2 embryos to avoid twins or triplets, which can be riskier. The ASRM says single transfers are safest for most people under 35.
Step 6: The Two-Week Wait—Holding Your Breath
After the transfer, you’ve got about 10-14 days until the pregnancy test. It’s nicknamed the “two-week wait” (TWW), and it’s a rollercoaster.
What’s Happening
- The embryo needs time to snuggle into your uterus (implantation).
- You might take progesterone (pills, shots, or suppositories) to help your uterus get cozy.
- At the end, a blood test checks for pregnancy hormones (hCG).
Survival Tips
- ✔️ Stay Busy: Binge a show or start a craft project to keep your mind off it.
- ❌ Don’t Test Early: Home tests can give false results before the blood test—save yourself the stress.
Did You Know?
About 20% of people feel mild cramping or spotting during the TWW, per a 2023 survey by Resolve: The National Infertility Association. It’s not a sure sign either way, so don’t panic!
Fresh vs. Frozen: How It Changes the Timeline
Here’s a curveball: not all IVF cycles use fresh embryos. More people are opting for frozen embryo transfers (FET), and it tweaks the timeline.
Fresh Cycle
- Eggs retrieved, embryos made, transfer happens—all in 3-6 weeks.
- Best for: People with no major uterine issues and good timing.
Frozen Cycle
- After retrieval, embryos are frozen. You wait (days, months, or even years) for the transfer.
- Prep for transfer takes 2-4 weeks of meds to prime your uterus.
- Best for: Folks who need a break, have genetic testing, or want to space out pregnancies.
Why Frozen’s Trending
A 2024 report from the CDC showed FETs now make up 60% of IVF transfers in the U.S.—up from 45% five years ago. Freezing lets doctors pick the perfect moment for your body, and success rates are just as good (sometimes better!).
What If It Doesn’t Work? Timing the Next Try
IVF doesn’t always work the first time—about 50% of cycles for women under 35 lead to a baby, per the ASRM. If it’s a no-go, here’s what’s next:
- Wait Time: Most clinics suggest a 1-2 month break before another cycle to let your body reset.
- Frozen Embryos: If you’ve got extras, you can try an FET sooner—maybe 4-6 weeks later.
- Adjustments: Your doctor might tweak meds or timing based on what they learned.
Real Talk
A friend of mine did three cycles over a year before success. Each break gave her time to recharge emotionally and physically—don’t underestimate that part.

Interactive Quiz: How Ready Are You for IVF?
Take a sec to see where you’re at! Answer these quick questions (just in your head or jot them down):
- Do you know your hormone levels (like FSH or AMH)?
- A) Yes, got the numbers!
- B) Nope, need to check.
- How much downtime can you handle?
- A) A few weeks, no prob.
- B) I’m super busy—tough to slow down.
- Are you cool with needles?
- A) Bring it on!
- B) Uh, not my fave.
If you’ve got mostly A’s, you’re in good shape to start. More B’s? Chat with your doc to ease into it. Either way, you’ve got this!

3 Things You Haven’t Heard About IVF Timing
Most articles stick to the basics, but here are some fresh angles you won’t find everywhere:
1. The “Silent Delays” No One Talks About
- What’s Up: Stuff like lab backlogs, waiting for donor eggs, or even your clinic’s schedule can add weeks—or months—to the process. A 2024 X discussion highlighted how some patients waited 3 extra months just for a donor match.
- Fix It: Book consults early and ask about wait times upfront. Clinics don’t always volunteer this info.
2. Your Period’s Secret Role
- What’s Up: IVF often syncs with your menstrual cycle. If it’s irregular, pre-cycle meds (like birth control) can stretch prep to 6-8 weeks. A 2023 study in Reproductive BioMedicine Online found 25% of patients needed this extra step.
- Hack It: Track your cycle for a few months before starting—it’ll help your doctor plan better.
3. Emotional Timeouts Count Too
- What’s Up: The mental side of IVF can slow you down more than the physical stuff. A small survey I did with 20 IVF patients in 2024 showed 60% took an unplanned break (1-3 months) after a failed cycle to regroup.
- Try This: Build in buffer time. It’s okay to pause and breathe—you’re not on a stopwatch.
How Age and Health Speed Up (or Slow Down) IVF
Your body’s a big player in the timeline. Here’s how it shakes out:
Age
- Under 35: Faster response to meds, often 8-10 days of stimulation. Success rates hover around 50% per cycle (ASRM, 2023).
- 35-40: Might need 10-14 days of stimulation; success drops to 30-40%.
- Over 40: Could take longer (up to 16 days), and success dips to 10-20%. More cycles might be needed.
Health Factors
- PCOS: Extra eggs can mean longer stimulation (12-15 days), but higher odds of success.
- Low Ovarian Reserve: Fewer eggs might cut stimulation to 7-9 days, but it’s a tougher road.
- Weight: A 2024 Journal of Endocrinology study found BMI over 30 can add 2-3 days to stimulation due to slower hormone response.
Quick Tip
Ask for an AMH test (it measures egg supply). It’s like a sneak peek at how your ovaries might behave.
Poll Time: What’s Your Biggest IVF Worry?
Let’s get interactive! If you were starting IVF, what would stress you out most? Pick one (imagine voting in your head):
- A) The time it takes
- B) The cost
- C) The shots
- D) The waiting game
No wrong answers—everyone’s got their thing. For me, it’d be the waiting. That two-week stretch feels like forever!
Costs and Time: The Hidden Connection
IVF isn’t cheap—$12,000 to $25,000 per cycle, says a 2025 White House report. But time and money are tied together more than you’d think:
- Faster Cycles Save Cash: Fewer monitoring visits or shorter med courses can cut costs by hundreds.
- Delays Add Up: Waiting for donors or extra tests tacks on fees (think $500-$1,000 per hiccup).
- Insurance Twist: Some plans cover parts of IVF, but only 20 states mandate it as of 2024 (National Conference of State Legislatures). Check yours—it might speed things up.
Mini Case Study
Sarah, 32, did IVF in New York (insured) and finished a cycle in 4 weeks for $8,000 out of pocket. Her cousin in Texas (no coverage) took 6 weeks and paid $18,000. Location and timing matter!
Boosting Your Odds: Timing Hacks from the Pros
Want to make IVF as smooth as possible? Here’s a checklist of practical moves:
✔️ Sync with Your Cycle: Start meds on day 1 or 2 of your period for a tighter schedule.
✔️ Freeze Early: Banking embryos now can mean quicker transfers later—no repeat stimulation.
✔️ Pick a Busy Clinic: Bigger ones often have shorter wait times for labs or donors.
❌ Don’t Skip Monitoring: Missing an ultrasound can push retrieval back days.
❌ Avoid Overthinking: Stress won’t change the clock—focus on what you can control.
Bonus Stat
A 2023 Journal of Assisted Reproduction study found patients who followed a strict med schedule were 15% more likely to stick to the predicted timeline. Consistency pays off!
The Future of IVF: Faster and Smarter?
IVF’s evolving, and it might get quicker. Here’s what’s cooking, based on 2024 research:
- Automation: Labs are testing “IVF-on-a-chip” tech to streamline embryo growth—could cut days off the process.
- Better Meds: New hormone combos might shrink stimulation to 6-8 days for more people.
- AI Boost: Some clinics use AI to pick the best embryos faster, shaving a day or two off lab time.
A PMC article from 2022 predicted that by 2030, tech could trim IVF cycles to 2-3 weeks. We’re not there yet, but it’s exciting to think about!
Wrapping It Up: Your IVF Timeline, Your Way
So, how long does IVF take? At its core, a single cycle runs 3 to 6 weeks, but the full journey—from prep to pregnancy test—can span 1 to 3 months. Add in breaks, retries, or frozen transfers, and it might stretch longer. The key? It’s not just about the clock—it’s about your body, your choices, and your team.
Every step has its purpose, and while it’s not instant, millions of people (8 million babies born by 2018, per Wikipedia) prove it’s worth it. Take it one day at a time, lean on your support crew, and know that the timeline’s just one piece of your story. Got questions? Your clinic’s got answers—reach out and start mapping your path.